Cerebra® S
Control Streptococcus suis
Trigger immune modulation
Streptococcus suis: A serious concern for pigs, producers and humans
Streptococcus suis (S. suis) was first reported in 1954 after outbreaks of meningitis, septicemia, and purulent arthritis among piglets (Hughes et al., 2009). Nowadays, it can still be seen as a major porcine pathogen. Infection with S. suis is one of the main causes of death during the post-weaning period from 5 to 10 weeks of age (Segura et al., 2016).
The pathogen
Streptococcus suis is an encapsulated, facultatively anaerobic, Gram-positive, α-hemolytic coccus. 35 serotypes (1-34 and ½) have been identified. Serotype 2 is considered the most common cause of the disease in Europe and worldwide.
S. suis is an emerging zoonotic pathogen of humans who come in contact with infected pigs or consume pork products that get contaminated with this pathogenic bacterium. Serotype 2 is the major zoonotic agent (Gottschalk et al., 2014).
Early life infection & latent carriage
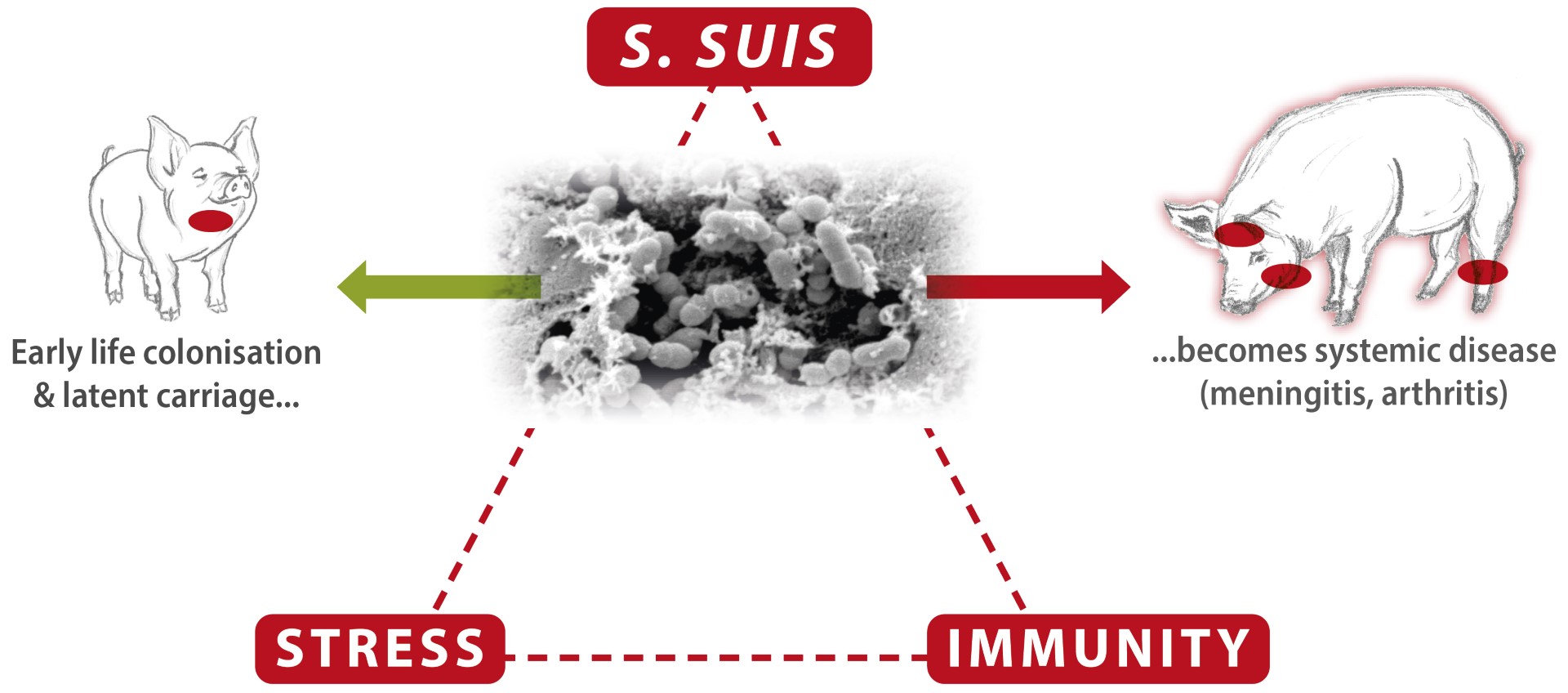
It is usually accepted that pigs’ main route of infection with S. suis is through the respiratory tract (oro-nasal) (Dekker et al., 2013). The pathogen is transferred from the sow’s vaginal secretions during parturition and the first days of life to the orо-nasal cavity of piglets and colonises their tonsils soon after birth (Gottschalk et al., 2003).
Horizontal transmission can also be part of the infection through contact with other herd members, especially during outbreaks (Segura et al., 2016).
After early life colonisation, the pathogen remains in the tonsils, while the infected pigs remain latent carriers without being sick. Therefore, the bacterium is already present in the herd and is waiting for predisposing factors that decrease immunity and contribute to disease occurrence (Cloutier et al., 2003, Gottschalk & Segura, 2019).
The role of the immune status and stress is crucial for the outbreak of S. suis infection
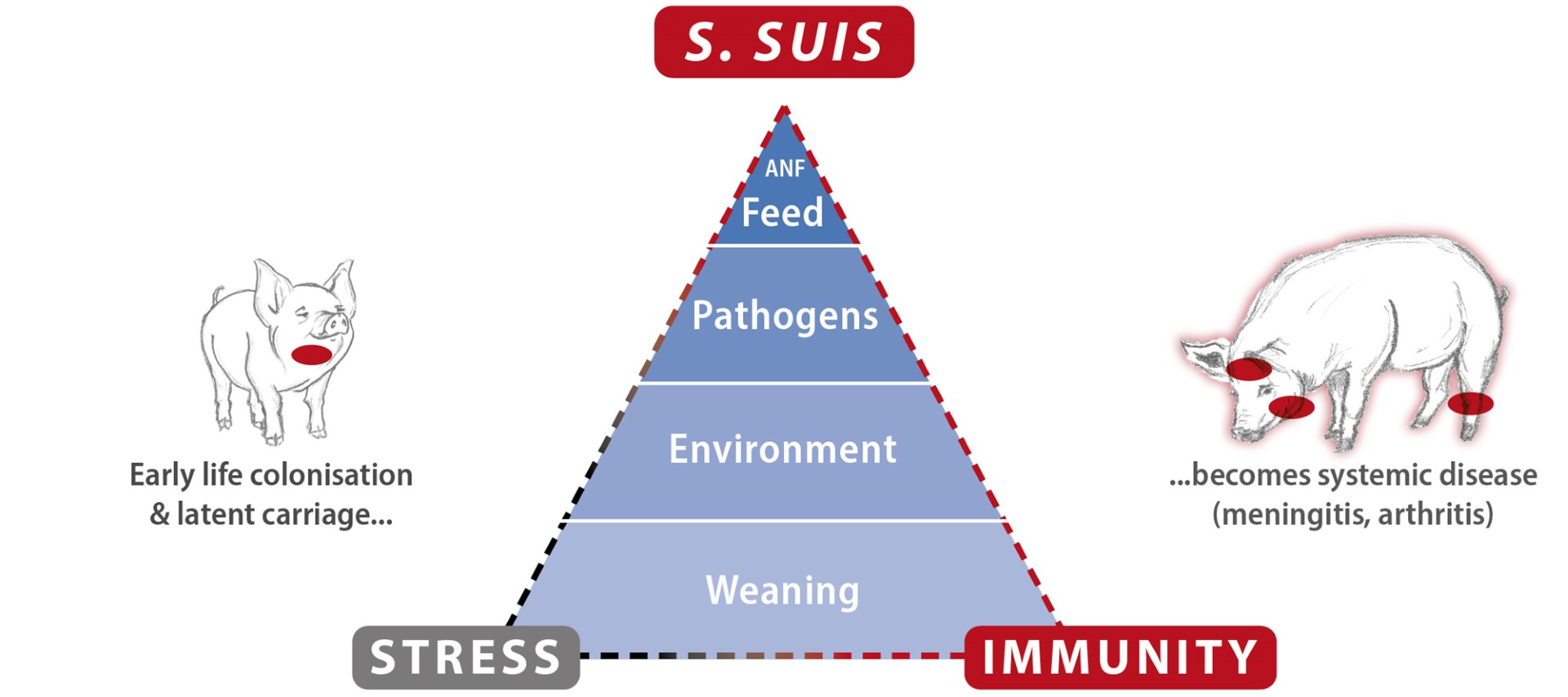
As S. suis is a facultative pathogen, different factors, both biotic (viral infections, for instance) and abiotic (such as weaning, ventilation problems and change of feed), can trigger its outbreaks (Seitz et al., 2016). The cumulating stress factors and inflammation during the pigs’ post-weaning/ transition period challenge the immunity mightily so that the threshold for keeping S. suis restricted can be exceeded. The pathogen penetrates mucosal barriers and occurs in the blood circulation, causing septicemia and organ dissemination, resulting in systemic disease, manifested with sudden mortality, central nervous symptoms (meningitis), joint problems (arthritis), and, less often, endocarditis and respiratory symptoms.
It is proven that S. suis outbreaks are exacerbated on farms positive to immunomodulatory viruses like PRRSv, and PCV2. The Swine influenza virus also contributes to the worsening of the situation. Hence, knowing the dynamics of these infections in each farm is very important.
Diagnosis and differential diagnosis
A presumptive diagnosis of S. suis infection is based on history, clinical signs, and gross lesions but requires laboratory confirmation. The proper sampling procedure is crucial to confirm or reject the diagnosis.
Differential diagnosis from other pathologies related to nervous symptoms like:
- Glaesserella parasuis
- Shiga-toxigenic Escherichia coli
- Sodium toxicity (high salt consumption or water deprivation)
- Phenylarsonic compound (organic arsenic) poisonings
- Aujeszky disease etc.
Differential diagnosis from other pathologies related to polyarthritis like:
- Mycoplasma hyorhinis
- Mycoplasma hyosynoviae
- Glaesserella parasuis
- Erysipelothrix rhusiopathiae
Control of S. suis outbreaks
The lack of an effective commercial vaccine to control and prevent S. suis infections and the controversial results of autogenous vaccines have promoted extensive prophylactic and metaphylactic treatments with a wide range of antimicrobial agents, such as penicillin, ampicillin, amoxicillin, or trimethoprim/sulfa, on farms (Varela et al. 2013; Seitz et al., 2016).
Despite the massive use of antimicrobials against S. suis and increased public health concerns about their resistance, some pigs become sick with often poor prognoses (Seitz et al., 2016).
Because of the specificity of the disease, S. suis requires prolonged antimicrobial treatment. In the field often, cases of lowering the doses can be observed. At the same time, sub-inhibitory concentrations of amoxicillin decrease its efficacy while increasing the S. suis inflammatory potential (Daniel Grenier et al., 2016).
According to the European Medicines Agency (EMA) Antimicrobial Expert Group (AMEG) Classification of WHO Critically Important Antimicrobials (CIAs) based on the level of risk to humans due to antimicrobial resistance development following use in animals, broad-spectrum penicillins are in the group with the highest threat to public health.
European legislation strongly emphasised the reduction of antimicrobial usage in relation to antimicrobial resistance. In 2022, new EU legislation prohibited all forms of routine antibiotic use in farming, including preventative group treatments.
All of the above put the effective control of Streptococcus suis outbreaks under a strong challenge.
To reduce antimicrobial use, S. suis disease prevention should concentrate on managing predisposing factors (stress) in combination with proper alternative treatment targeting Gram+ bacteria and strong immunity support of the animals, especially during the stressful post-weaning/transition period.
Cerebra® S
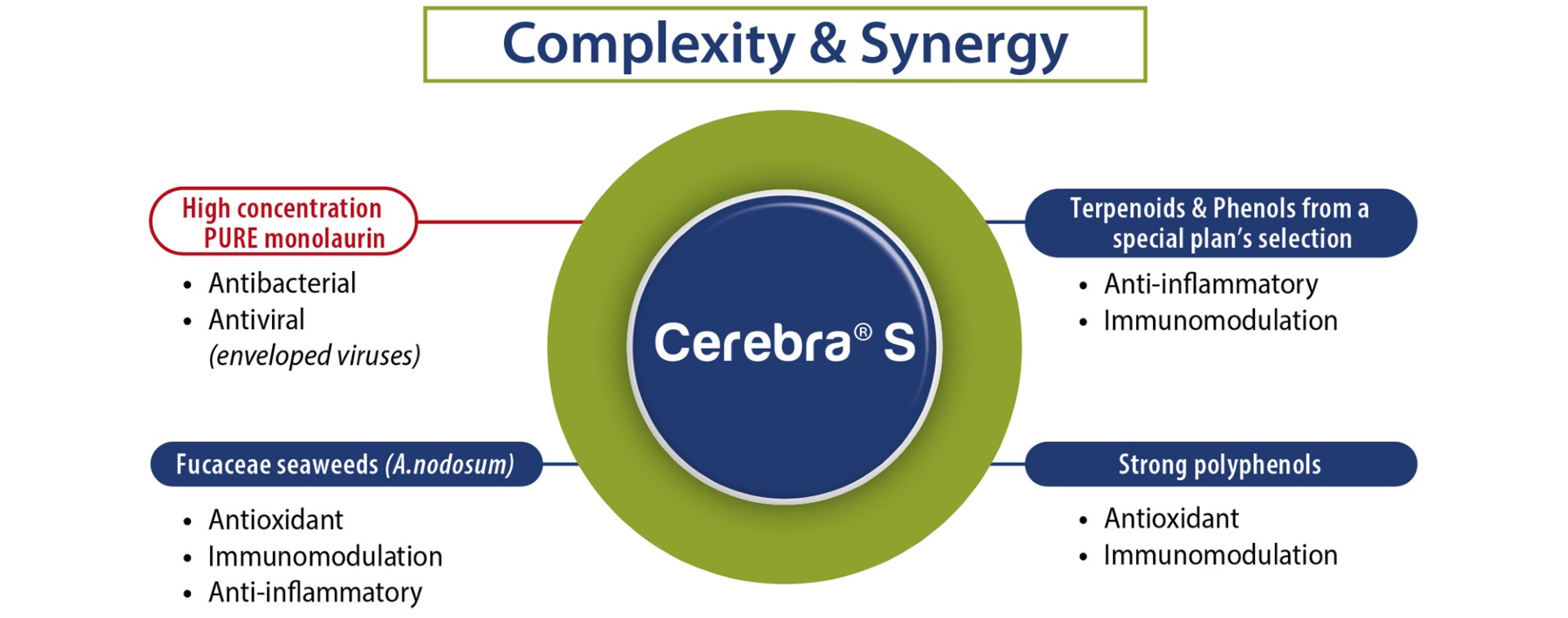
Thanks to the precise selection of specific ingredients, Cerebra® S is:
- Efficient against Gram (+) bacteria
- Ensuring strong immunity & antioxidative support
- Reducing medication
Application program
Due to the specificity of the disease, the recommendation of Innovad's S. suis control program is based on an assessment of the condition of each farm after completing Innovad’s checklist. Please contact Dr. Milena Sevastiyanova, DVM – INNOVAD Global Technical Lead (m.sevastiyanova@innovad-global.com), to request the checklist.

If you have any questions, please do not hesitate to contact Dr Milena Sevastiyanova, DVM – INNOVAD Global Technical Lead (m.sevastiyanova@innovad-global.com).
Product composition and positioning may vary by market based on the regulatory status.
